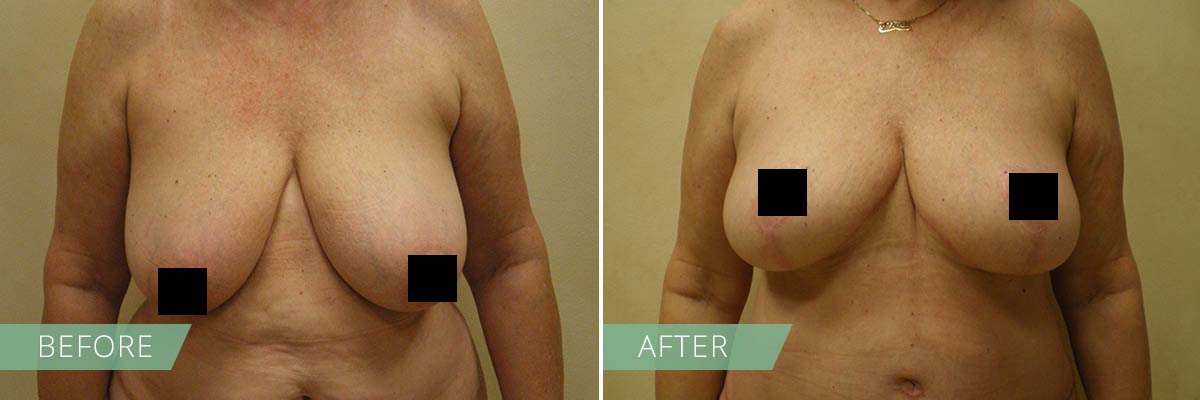
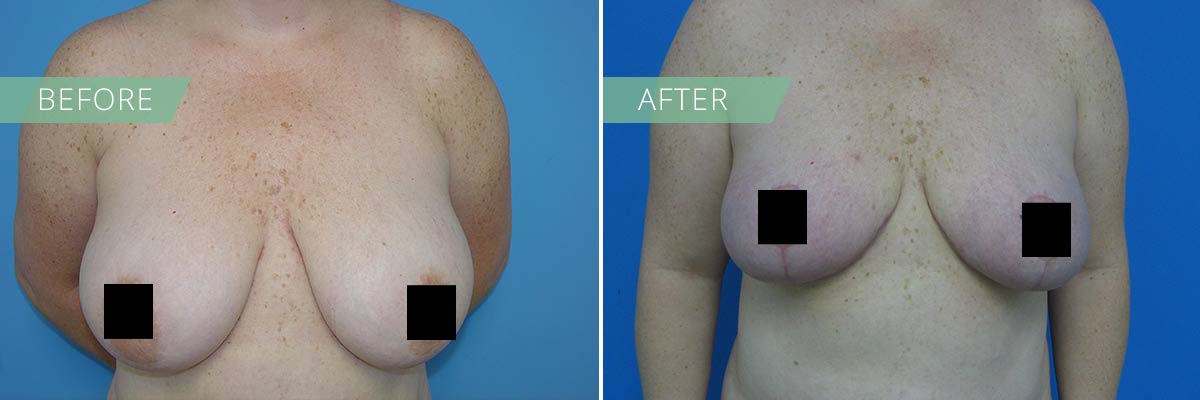
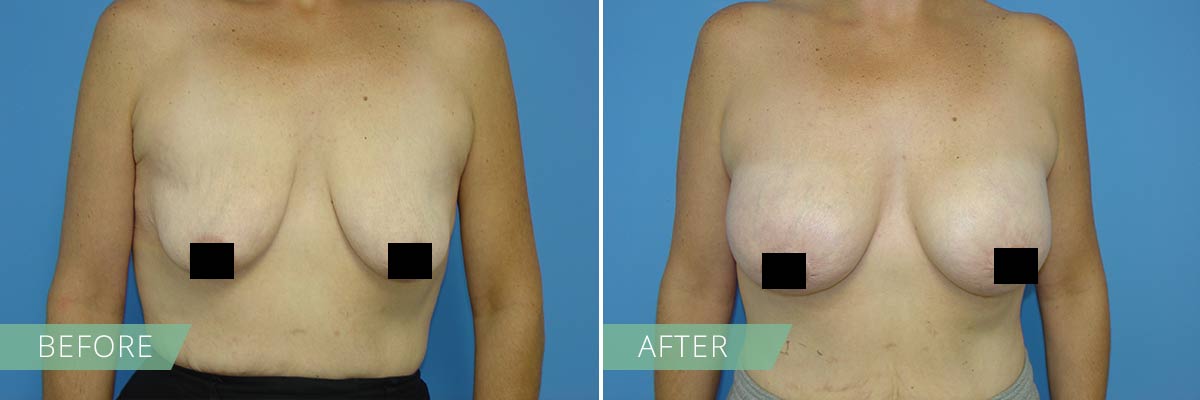
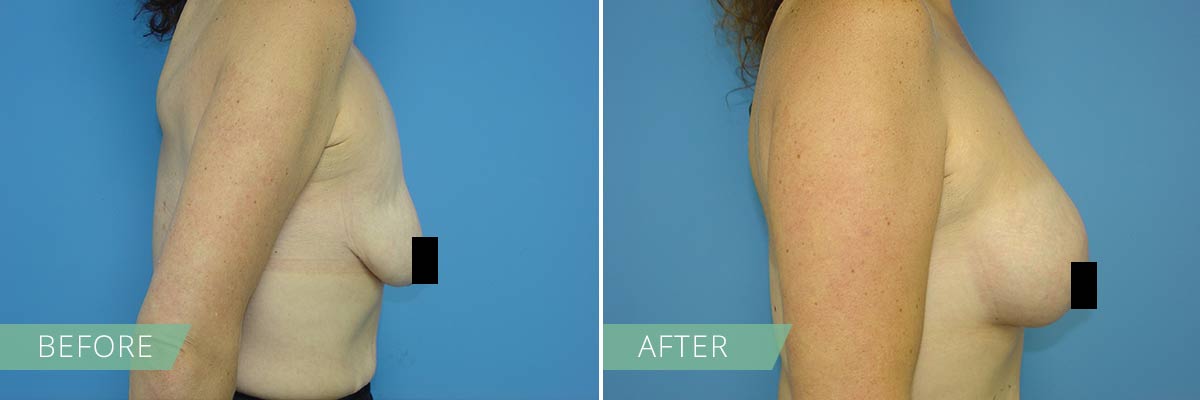
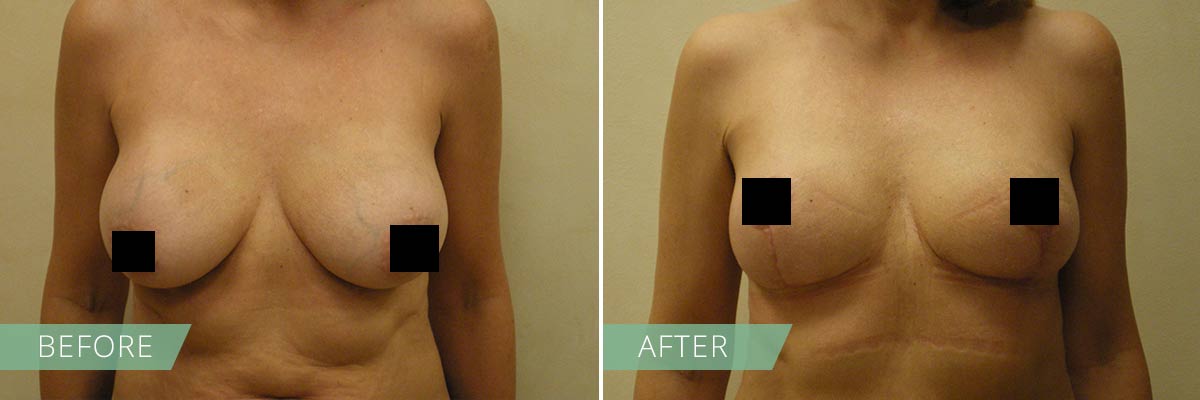
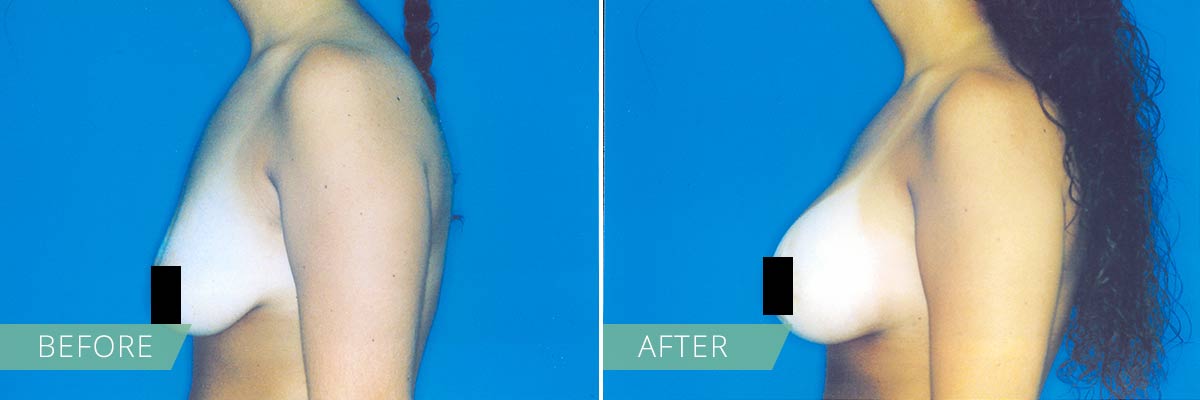
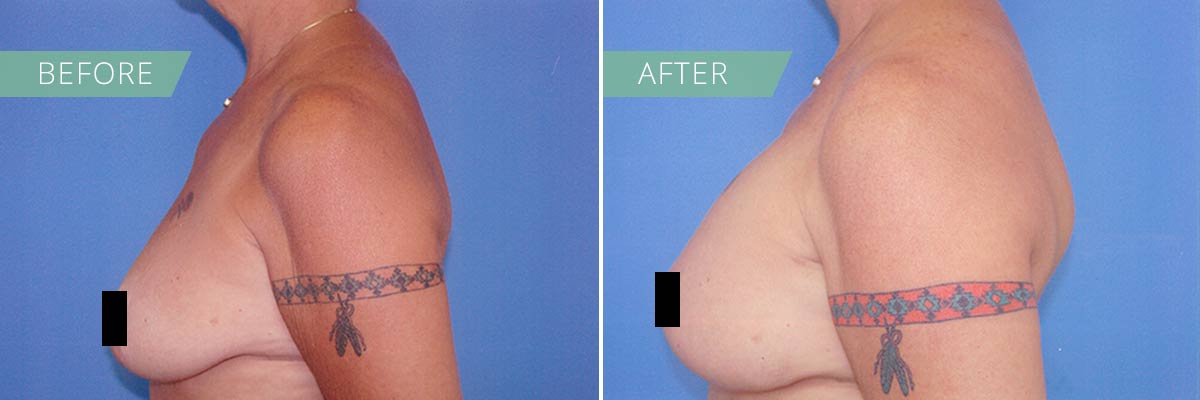
If you desire to restore the firmness and shape of your breasts, then a breast lift may be right for you. In general, breasts lift raises and firms the breasts by removing excess skin and tightening the surrounding tissue to reshape and support the new breast contour. Sometimes the areola (the pigmented skin surrounding the nipple) has become enlarged over time, and a breast lift will reduce this as well. A breast lift rejuvenates the female figure with a breast profile that is more youthful, uplifted and firm.
Breast lift, technically called mastopexy, is surgery to uplift and improve the shape of a female breast that:
- Sags or is pendulous, but is proportionate with the body frame
- Has lost firmness and skin elasticity
- Has a flatter, elongated shape
- When unsupported, the nipple falls below the breast crease
- Has a nipple and areola (the pigmented skin surrounding the nipple) that point downward
- Has stretched skin and an enlarged areola
A breast lift is appropriate for women who wish to improve breast shape and position. When an increase in breast volume is also desired, Breast Implants may be inserted in conjunction with a breast lift.
While South Florida Breast Surgery does not generally affect breast function, women who are planning future pregnancies, should discuss this with Dr. Yalamanchi. The changes that occur in the breast during pregnancy can minimize or reverse the improvement of a breast lift that it provides. Likewise, plans for significant weight loss, should also be discussed. For these reasons, good candidates for a breast lift are generally women of normal, stable weight whose breasts are fully developed. Breast lift is appropriate in younger women, as well, most commonly, is cases of breast asymmetry where the position of one breast is lower than the other.
A breast lift is best performed on:
- Healthy individuals who do not have a life-threatening illness or medical conditions that can impair healing
- Non-smokers
- Individuals with a positive outlook and specific goals in mind for body image
Overall health and personal outlook can greatly impact the outcome of breast lift surgery. These will be carefully evaluated in your consultation. The success of your procedure, safety and overall satisfaction require that you:
- Honestly share your expectations with Dr. Yalamanchi
- Fully disclose health history, current medications, the use of vitamins, herbal supplements, alcohol, tobacco, and drugs
- Be candid about any history of breast cancer in your family and your personal breast health
- Commit to precisely following all of the instructions
Breast lift is a highly individualized procedure achieved through a variety of incision patterns and techniques. The appropriate technique for your case will be determined based on:
- Breast size and shape
- The size and position of the areola
- The degree of breast sagging
- Skin quality and skin elasticity as well as the amount of extra skin
There are many variations to the procedure however; one of the most common is a pattern with three incisions:
- Around the areola
- Vertically down from the areola to the breast crease
- Horizontally along the breast crease
Through these incisions, the underlying breast tissue is lifted and reshaped to improve breast contour and firmness. The nipple and areola are repositioned to a natural, more youthful height. If necessary, enlarged areolas are reduced by excising skin at the perimeter. Excess breast skin is removed to compensate for a loss of elasticity.
Alternative techniques eliminate either the horizontal incision at the breast crease, the vertical incision from the areola to the breast crease or sometimes both. In any case, incisions are usually placed so that they can be hidden under clothing and swimsuits. Non-removable sutures are layered deep within the breast tissue to create and support the newly shaped breasts. Sutures, skin adhesives and/or surgical tape, may be used to close the skin.
Incision patterns for a breast lift are determined based on the amount of excess skin, skin elasticity and the degree of lift necessary to achieve realistic goals. The incisions may include a circle around the areola, a line extending down the lower portion of the breast from the areola to the crease underneath the breast and a line along the crease under the breast. Not all women will require all of these incisions. It is possible to perform a breast lift through an incision around the areola only, or through a combination of incisions around the areola down the lower portion of the breast. More commonly, three incisions including one along the breast crease are used. The combination, length, and extent of incisions depend on the amount of excess skin to be removed and the quality of the skin.
Once the excess skin is removed, the breast tissue is reshaped and lifted, and the remaining skin tightened, as the incisions are closed. Some incision lines resulting from breast lift are concealed in the natural breast contours; however, others are visible on the breast surface. Incision lines are permanent, but in most cases, will fade and significantly improve in appearance over time. Your more youthful and uplifted breast profile, and an enhanced body image, should bring you great satisfaction.
Possible risks of breast lift include blood pooling, beneath the skin (hematoma), infection, or poor healing at the incision site, and changes in nipple or breast sensations, that are usually temporary. Any surgery carries risks associated with anesthesia. These and others risks will be fully discussed prior to your consent.
Following surgery
Once your procedure is completed, dressing or bandages will be applied to your incisions, and an elastic bandage or support bra will minimize swelling and support the breast as they heal. A small, thin tube may be temporarily placed under the skin to drain any excess blood that may collect. Before your released following surgery, you and an accompanying family member, friend or caregiver will be given specific instructions that may include:
- How to care for the breast
- Medications to apply or take orally to aid healing and reduce the of infection
- Specific changes at the surgical site or in overall health
- When to come back for follow up visits
Initial healing will include swelling, discomfort at the incision site. Discomfort is common and can be controlled with medication. a support bra may be recommended around the clock for the first week or two. It is important to cleanse the incision sites and apply ointment as directed. Follow all instructions carefully; this is essential to the success of your outcome. A return to light, normal activity is possible as soon as you feel ready, usually within a few days of surgery.
Initial wound healing may take from 5 to 10 days, at which time any sutures will be removed. You will be ready to return to work and normal activity at this time, so long as you do not engage in any heavy lifting or vigorous exercise.
Healing will continue for several weeks, as swelling dissipates and incisions lines continue to improve. Continue to follow the instructions and attend follow-up visits as scheduled.
The final results of your breast lift will appear over the next few months as breast shape and position continue to settle. Incision lines are permanent, but they most likely won’t be visible even under your favorite bathing suit.
Over time, your breast can continue to change due to aging and gravity. Your new breast profile is best maintained by maintaining your weight, a healthy lifestyle and proper support of your now firm and rejuvenated breasts.
BREAST RECONSTRUCTION
The goal of breast reconstruction is to create a soft, natural-looking breast for a woman who must undergo breast removal, due to cancer or other diseases. Whether it is performed immediately following a mastectomy or at a later time, breast reconstruction can dramatically improve a woman’s appearance, self-confidence and overall quality of life.
Almost every woman who has lost a breast to cancer can have her body restored with breast reconstruction. However, the following conditions are desirable:
- You clearly understand that although your figure will be markedly improved, your reconstructed breast will not look or feel exactly the same, as the breast that was removed
- Your oncologist has advised you that reconstruction is appropriate for you with regard to your stage of cancer or treatment. (Should cancer recur, your reconstructed breast will not interfere with further treatment. However, such treatment may affect the appearance of your reconstructed breast.)
- You may feel that you are able to handle the period of emotional adjustment that may accompany breast reconstruction. Just as it takes time to get use to the loss of a breast; it may take some time before you begin to think of the reconstructed breast as your own
- You have no additional health concerns that may complicate the procedure, such as obesity or heart disease
There are many options available for breast reconstruction. Your anatomy, Dr. Yalamanchi’s preferences and your desired results will help determine which method is best for you. The most common method of reconstructing a breast is skin expansion with a breast implant. Following a mastectomy, a balloon expander is inserted beneath the skin and cheek muscle. Over several weeks, the expander balloon is gradually filled with a salt-water solution in the doctor’s office, causing the overlying skin to stretch. When the skin had stretched sufficiently, the expander is surgically replaced with a more permanent implant. Some expanders are designed to be left in place as the final implant. The nipple and the skin surrounding it, called the areola, are reconstructed in a later procedure. In rare cases, when a sufficient amount of skin is available, an implant can be placed without the preliminary skin-expansion step.
The Flap reconstruction method is more involved at the initial procedure than reconstruction with an implant, however many women prefer it, because it may allow the breast to be rebuilt with natural tissue. Also, unlike the tissue expander method, the breast mound is completed at the initial operation, without the need for expansion over an extended time period.
In one method, the breast is reconstructed using a tissue flap – consisting of a portion of skin, fat, and muscle – that is taken from the back, or abdomen. The flap, still tethered to its original blood supply, is tunneled beneath the skin to the front of the chest wall. The transported tissue may be bulky enough to create a new breast mound itself. However, sometimes an implant will be inserted as well.
- A tissue expander is inserted following the mastectomy to prepare for reconstruction
- The expander is gradually filled with saline through an integrated or separate valve to stretch the skin enough to accept an implant beneath the chest muscle
- After surgery, the breast mound is restored. Scars are permanent, but will fade with time. The nipple and areola are reconstructed at a later date
- The transported tissue is used to cover the implant and replace skin deficit
- The flap is being placed over the breast implant
- The transported tissue forms a flap for a breast implant or it may provide enough bulk to form the breast mound without an implant
- Tissue may be taken from the abdomen and tunneled to the breast or surgically transplanted to form a new breast mound
- After surgery, the breast mound, nipple, and areola are restored
- Scars at the breast, nipple, and abdomen will fade substantially with time, but may never disappear entirely. In a more complex flap technique, tissue that is removed from the abdomen is surgically transplanted to the chest by reconnecting the flap’s blood vessels to vessels in the chest region
Although more complicated, this microsurgical reconstruction may provide a more natural and less traumatic reconstruction in many women. Even though recovery from flap reconstruction may take longer than with implant reconstruction at the initial procedure, it does not require a secondary procedure for placing a permanent implant, nor does it require the weekly office visits needed for tissue expansion. Additionally, a flap procedure may improve the contour of the site from which the borrowed tissue was taken. For example, a protruding abdomen may appear trimmer after tissue is taken from the area and used to rebuild the breast.
All of these procedures have advantages and disadvantages, and many times the choice of procedure is limited by other health factors, such as weight, other medical conditions and previous cancer therapy. Dr. Yalamanchi will help you to determine which procedure is best for you.
Follow-up procedures
Once the breast mound is restored in the initial procedure, one or more follow-up procedures will be performed to replace a tissue expander with a permanent implant or to reconstruct the nipple and areola. Dr. Yalamanchi may also recommend an additional operation to lift or reduce the opposite breast to match the appearance of the reconstructed breast.
Each year, thousands of women undergo breast reconstruction and experience no major complications. However, one on the most important parts of your consultation with Dr. Yalamanchi is discussing the risks, as well as, the potential benefits of surgery. Certain complications are possible in any type of surgery including; blood loss, and infection. Your specific risks will be discussed.
Potential complications specific to breast reconstruction, vary with the type of reconstruction you and Dr. Yalamanchi choose. For instance, with flap reconstruction, there is a small risk of partial or, very rarely, complete flap loss. Reconstruction with an implant had the potential for breast firmness (capsular contracture) and implant rupture. The probability of having one of these, or other complications, must be thoroughly discussed with Dr. Yalamanchi.
Remember, by carefully following Dr. Yalamanchi’s instructions – both before and after surgery – you can do your part to minimize some of the risks.
What can I expect on the day of my surgery?
Breast reconstruction usually involves more than one operation. The first stage, whether performed at the same time as the mastectomy, or later, is typically performed in a hospital. Follow-up procedures may be performed in a hospital, an outpatient surgery center or an office-based surgical suite.
Medications are administered to keep you comfortable during the procedure. Usually a general anesthetic is used in the first procedure to reconstruct the breast mound so that you will sleep throughout the entire surgical procedure. Follow-up procedures may require only local anesthesia. We will discuss the types of comfort measures that will work best for you.
How will I look and feel right after surgery?
When surgery is complete, you’ll be taken to a recovery area. Small drainage tubes may have been placed beneath the skin near the surgical sites to help prevent fluids from accumulating. Recovering from a combined mastectomy, and reconstruction surgery, or from a flap reconstruction, typically takes longer, than recovery from an implant reconstruction, or a reconstruction performed apart from the mastectomy. Although everyone heals at a different rate, your recovery may follow this general time line:
Within the first week:
- Surgical drains (if used) will be removed and dressings will be changed
- Your stitches will be removed
After two weeks:
- Any lingering soreness at the surgical sites will diminish
- You will feel less fatigued and have more energy
After several weeks:
- You may return to most of your normal activities, including sports and sexual activity
- You may begin stretching & exercising, which may be recommended by Dr. Yalamanchi
- Your scars will begin to fade, although, it may take many months to see substantial fading
Sensation may return to some areas of the breast. However, a reconstructed breast will never feel completely normal or have normal sensation.
What should I know about my results?
If you are like most women who undergo breast reconstruction, you will find that the procedure provides both physical and emotional rewards. For many women, breast reconstruction represents a new start, the change to put breast cancer behind them, and get on with their lives. You should expect to go through a period of adjustment to your new look. However, any concerns about your new shape are likely to pass within a few months, as you begin to think of the reconstructed breast (s) as your own.